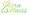Introduction
Menopause is a significant transition in a woman's life, and it often brings a wave of physical changes that can be quite uncomfortable, especially when it comes to knee pain. As estrogen levels dip, many women find themselves grappling with increased inflammation and joint discomfort, making even the simplest daily activities feel overwhelming.
We understand how daunting this phase can be. You are not alone in feeling this way. Many women share these struggles, and it’s important to acknowledge the emotional and physical toll it can take. But there’s hope. This article explores essential strategies to manage knee pain during menopause, offering practical steps that can truly enhance your overall well-being and mobility.
Imagine navigating this challenging time while still maintaining an active lifestyle, minimizing discomfort, and feeling empowered. We are here to help you find that balance.
Understand the Link Between Menopause and Knee Pain
Menopause can be a challenging time for many women, and the hormonal changes that come with it, especially the drop in estrogen, can lead to stiffness and discomfort. We understand how vital estrogen is for maintaining the health of connective tissues, as it helps regulate inflammation and influences how we perceive discomfort. As estrogen levels decrease, many women find that their joints, particularly in the lower limbs, become more uncomfortable due to increased inflammation and the wear and tear of cartilage. Research shows that estrogen's anti-inflammatory properties can help keep inflammatory factors in check, which often spike during this transition.
Common menopause symptoms, like weight gain and decreased physical activity, can further intensify joint discomfort. Gaining weight puts extra stress on your limbs, while being less active can lead to muscle weakness and stiffness, making it even harder to manage discomfort in your legs. Additionally, the natural changes during this time, such as losing muscle strength and gaining fat, can contribute to the onset of [knee osteoarthritis](https://misrawellness.com) (KOA).
Inflammation is a significant player in joint discomfort, and this transition can elevate inflammatory markers in your body. The decline in estrogen is linked to higher levels of pro-inflammatory cytokines, which can worsen discomfort and stiffness in your limbs. Understanding these inflammatory processes is essential for creating effective strategies to manage knee pain associated with menopause and knee pain during this stage of life.
At Misra Wellness, we recognize that each woman's health journey is unique. We take into account your personal health history, including any pre-existing joint conditions, when crafting management strategies. If you have a history of joint issues, you might experience more intense symptoms during this transition, which is why a tailored approach to treatment is so important. By understanding how hormonal changes, weight management, physical activity, and inflammation interact, you can better navigate the challenges of menopause and knee pain.
Engaging in regular aerobic exercise for 40 minutes, five times a week, has been shown to significantly alleviate discomfort associated with knee osteoarthritis. This practical approach can make a real difference in managing your symptoms. Additionally, we offer medical weight loss options when appropriate, ensuring you receive comprehensive support for your weight and overall health. Remember, you are not alone in this journey, and we are here to help.
Incorporate Regular Exercise and Healthy Eating Habits
Incorporate Regular Exercise and Healthy Eating Habits
We understand that managing menopause-related joint pain can be challenging, and it’s essential to find ways to enhance your overall well-being during this time. At Misra Wellness, we’re here to support you with personalized care tailored to your unique needs. Let’s explore some strategies that can make a difference:
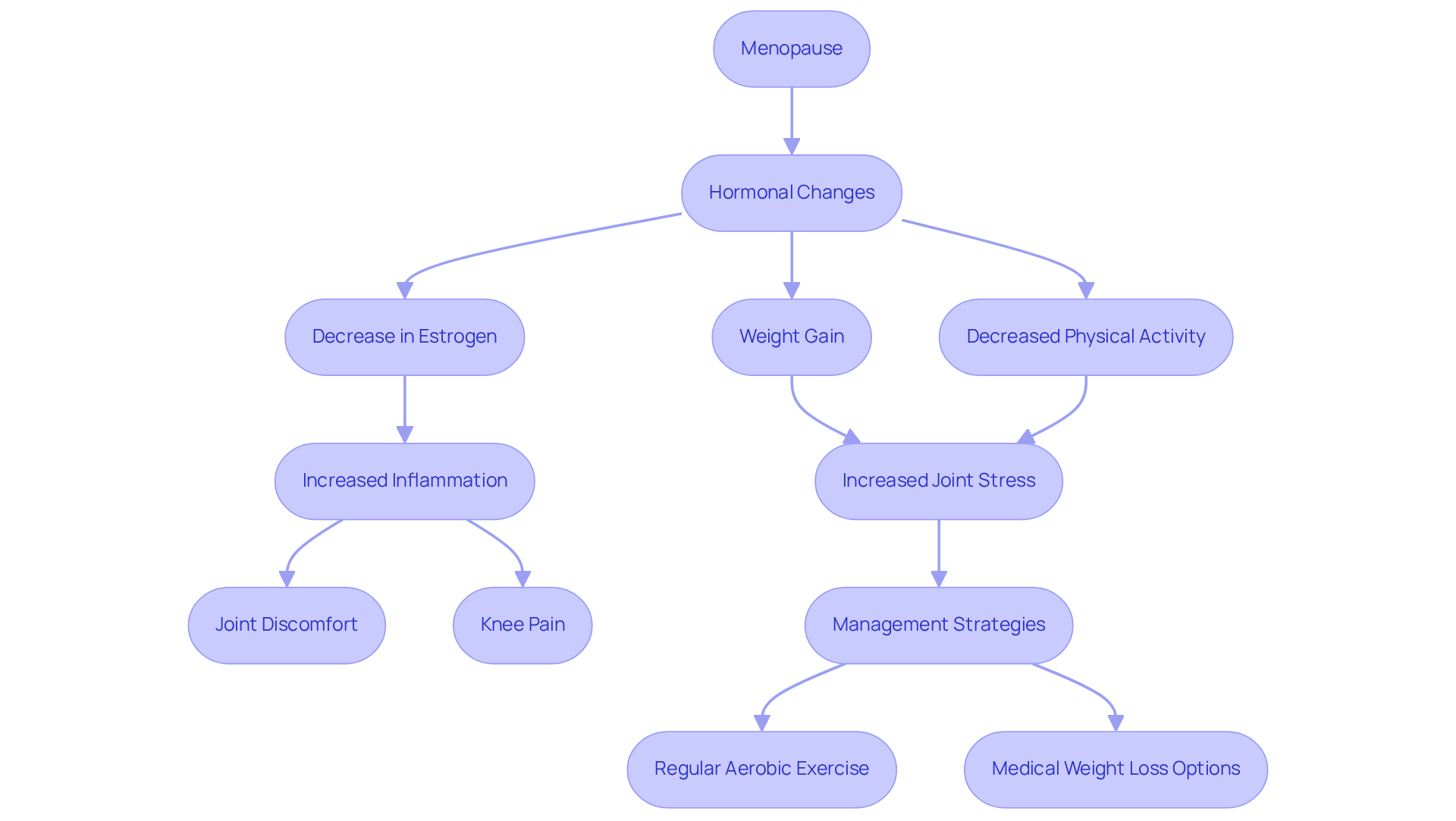
- Strength training: Prioritize exercises that strengthen the muscles around your knees, like squats and leg lifts. Engaging in 2-4 strength training sessions each week can help preserve and build muscle mass, which is crucial as estrogen levels decline during menopause and can also help alleviate knee pain. As Dr. Christina DeAngelis wisely points out, "People underestimate how powerful it is" when it comes to strength training for women in midlife.
- Low-impact cardio: Activities such as swimming, cycling, or brisk walking can support your cardiovascular health while being gentle on your body. These exercises not only help manage knee pain but also support individuals dealing with menopause and knee pain, improving your overall fitness.
- Flexibility exercises: Incorporating stretching or yoga can enhance your mobility and alleviate stiffness. Mind-body exercises can also help manage stress, which is so important during this stage of life. Experts recommend adding balance exercises, like tai chi or simply standing on one leg, to prevent falls that could lead to injuries.
In addition to exercise, embracing an anti-inflammatory diet can significantly support your joint health:
- Fruits and vegetables: Aim for a colorful variety to ensure you’re getting a broad spectrum of nutrients that support your overall health.
- Healthy fats: Incorporate sources like avocados, nuts, and olive oil, which can help reduce inflammation.
- Lean proteins: Choose fish, poultry, and plant-based proteins to support your muscle health and recovery.
By incorporating these strategies, you can significantly enhance your joint health and overall well-being during this phase of life, especially in managing menopause and knee pain, while addressing both the physical and emotional aspects of your health. At Misra Wellness, we offer tailored care plans for women navigating this life stage, including [nutritional guidance](https://misrawellness.com) and holistic support. We want to ensure you have the resources needed to thrive during this transitional phase. Remember, prioritizing recovery time and mindfulness activities can further enrich your fitness journey.
Consult Healthcare Providers About Treatment Options
It's important to arrange regular check-ups with a healthcare provider who understands the unique challenges of this stage of life. Consider reaching out to someone like Dr. Misra at Misra Wellness, who offers comprehensive care tailored to your individual needs.
You might be feeling overwhelmed by discomfort during menopause and knee pain, especially related to joint pain. You're not alone in this journey, and there are options available to help you find relief. Let’s explore some potential treatment paths together:
- Hormone Replacement Therapy (HRT): This option can be a game-changer for many. It’s worth evaluating the benefits and risks of HRT as part of a personalized menopause care plan. Research indicates that both past and current users of hormone therapy have experienced a lower prevalence of osteoarthritis in the legs, suggesting a protective effect. Estrogen may help prevent cartilage damage and reduce knee deterioration, making it a viable choice for managing discomfort associated with menopause and knee pain.
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Over-the-counter options can provide relief, but it’s essential to be aware of the risks. While NSAIDs are commonly used by menopausal women, prolonged use can increase the chances of falls and gastrointestinal bleeding, particularly in older adults. Despite these concerns, they remain a popular choice, with about 26% of individuals over 60 using them for relief.
- Supplements: You might also want to explore supplements like glucosamine, chondroitin, or turmeric. These can offer additional support for joint health and help manage discomfort.
Keeping a symptom diary can be incredibly beneficial. By tracking your discomfort levels, triggers, and any other health changes, you can provide your healthcare provider with valuable insights. This holistic approach ensures that your care is as effective as possible. Remember, we are here to help you navigate this journey.
Track Symptoms and Progress for Effective Management
We understand that dealing with menopause and knee pain, along with discomfort in your joints, can be incredibly challenging. It’s not just about the physical pain; it’s about how it affects your daily life and well-being. That’s why we encourage you to consider using a symptom tracker. This simple tool can help you record your daily experiences and gain insights into your health.
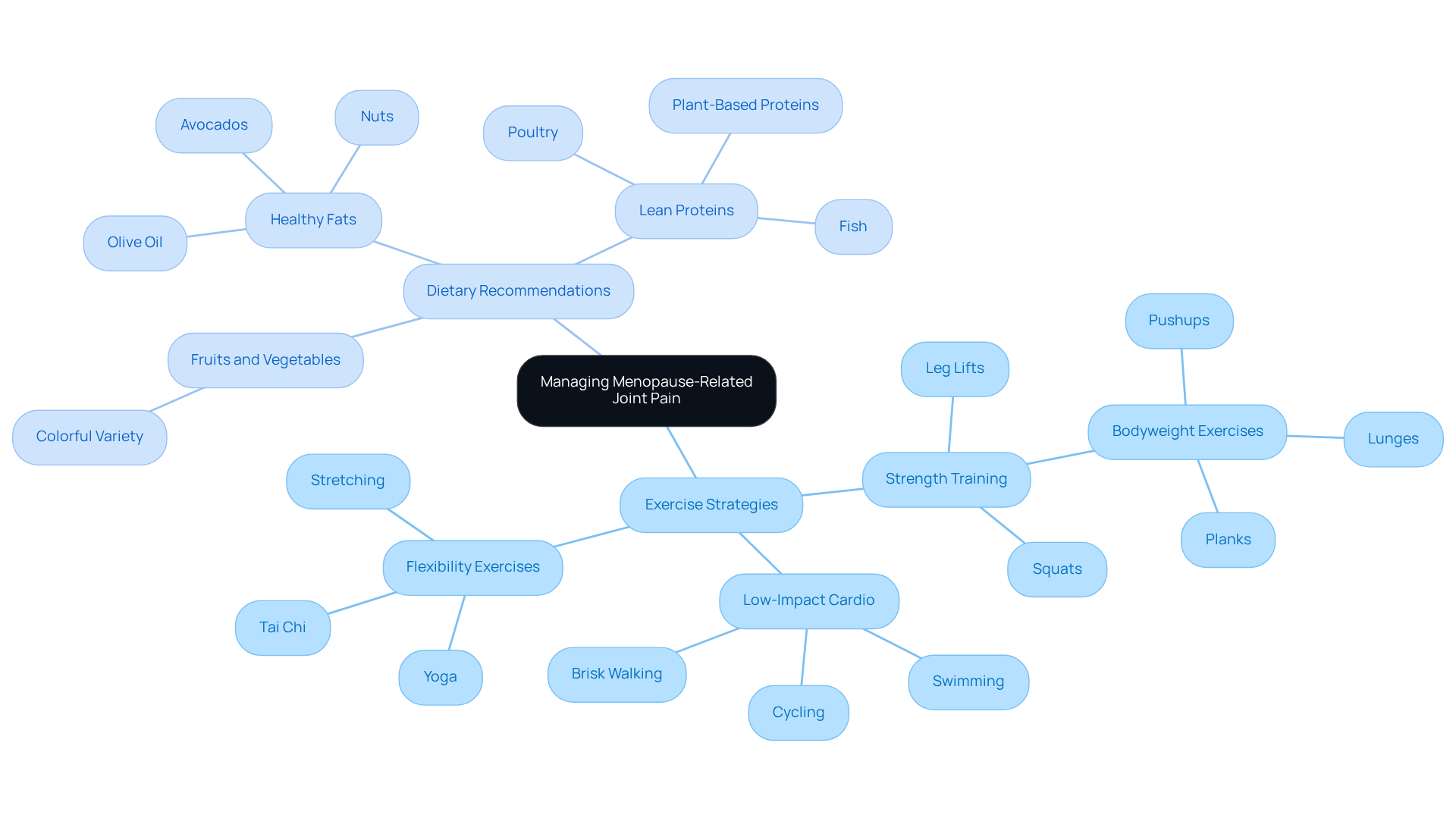
Start by noting your pain intensity. Rate your pain on a scale from 1 to 10. This can help you identify fluctuations and triggers, giving you a clearer picture of what you’re experiencing. Next, pay attention to your activity levels. Record the types and durations of physical activity you engage in, and observe how different exercises impact your knee discomfort. Lastly, don’t forget about your dietary habits. Keeping track of what you eat, especially focusing on anti-inflammatory foods, can make a significant difference in alleviating your symptoms.
Regularly reviewing your tracker can reveal patterns that you might not have noticed before. This is a powerful step in your journey. Discuss your findings with your healthcare provider during appointments. By sharing this information, you can work together to adjust your management plan based on what the data shows. This proactive approach can lead to strategies that yield the best results for you.
It’s important to remember that you are not alone in this. Studies indicate that over 40% of women experience muscle or joint pain, including menopause and knee pain, during the transition to menopause. Effective symptom management is crucial, and we are here to help you navigate this journey.
Conclusion
Menopause can be a challenging time for many women, especially when it comes to dealing with knee pain. The hormonal changes, particularly the drop in estrogen, can lead to increased inflammation and discomfort in the joints. We understand how overwhelming this can feel, and recognizing this connection is vital for finding ways to ease the pain and enhance your quality of life during this transition.
To help manage knee pain during menopause, consider incorporating the following:
- Regular exercise
- Embracing healthy eating habits
- Consulting with healthcare providers for personalized treatment options
Engaging in strength training, low-impact cardio, and flexibility exercises can significantly improve joint health. Additionally, an anti-inflammatory diet can support your overall well-being. Tracking your symptoms and progress can empower you to take a proactive approach, allowing you to adjust your strategies as needed.
Remember, you don’t have to navigate the journey through menopause and its accompanying knee pain alone. By utilizing available resources, seeking professional guidance, and committing to a comprehensive management plan, you can face this life stage with confidence and resilience. Embracing these essential steps not only helps you take control of your health but also enhances your ability to thrive during this significant transition. We are here to help you every step of the way.
Frequently Asked Questions
How does menopause affect knee pain?
Menopause leads to hormonal changes, particularly a drop in estrogen, which can cause stiffness and discomfort in joints, especially in the lower limbs. This is due to increased inflammation and wear and tear of cartilage as estrogen levels decrease.
What role does estrogen play in joint health during menopause?
Estrogen is vital for maintaining the health of connective tissues, regulating inflammation, and influencing pain perception. Its decline during menopause can lead to increased inflammatory factors that worsen joint discomfort.
What are common menopause symptoms that can exacerbate knee pain?
Common symptoms include weight gain and decreased physical activity, which can increase stress on joints, lead to muscle weakness, and contribute to stiffness, making it harder to manage knee pain.
How does inflammation relate to knee pain during menopause?
The decline in estrogen is linked to higher levels of pro-inflammatory cytokines, which can elevate discomfort and stiffness in the joints. Understanding these inflammatory processes is crucial for managing knee pain effectively.
What strategies can help manage knee pain associated with menopause?
Engaging in regular aerobic exercise for 40 minutes, five times a week, can significantly alleviate discomfort associated with knee osteoarthritis. Additionally, tailored management strategies considering personal health history can be beneficial.
What should women consider if they have a history of joint issues during menopause?
Women with a history of joint conditions may experience more intense symptoms during menopause, making it important to have a tailored approach to treatment that addresses their unique health needs.
What support options are available for managing weight during menopause?
Medical weight loss options may be offered when appropriate, providing comprehensive support for weight management and overall health during menopause.
How can women navigate the challenges of menopause and knee pain?
By understanding the interplay of hormonal changes, weight management, physical activity, and inflammation, women can better navigate the challenges associated with menopause and knee pain.
List of Sources
- Understand the Link Between Menopause and Knee Pain
- The Mechanism by Which Estrogen Level Affects Knee Osteoarthritis Pain in Perimenopause and Non-Pharmacological Measures - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11942494)
- Menopause and Joint Pain: An Orthopedic Perspective (https://orthopedicsri.com/blog-items/menopause-and-joint-pain-an-orthopedic-perspective)
- Understanding Menopause’s Impact on Musculoskeletal Health | Duke Department of Orthopaedic Surgery (https://ortho.duke.edu/news/understanding-menopauses-impact-musculoskeletal-health)
- Inflammation, menopause and hormones: what’s the connection? (https://drlouisenewson.co.uk/knowledge/inflammation-menopause-and-hormones-whats-the-connection)
- The Mechanism by Which Estrogen Level Affects Knee Osteoarthritis Pain in Perimenopause and Non-Pharmacological Measures (https://mdpi.com/1422-0067/26/6/2391)
- Incorporate Regular Exercise and Healthy Eating Habits
- How to Exercise Effectively in Perimenopause and Menopause (https://news.umiamihealth.org/en/how-to-exercise-effectively-in-perimenopause-and-menopause)
- Strength training tied to smaller risk of knee osteoarthritis and pain later in life - Harvard Health (https://health.harvard.edu/diseases-and-conditions/strength-training-tied-to-smaller-risk-of-knee-osteoarthritis-and-pain-later-in-life)
- Strength training is crucial after menopause. How to make the most of your workouts (https://apnews.com/article/menopause-perimenopause-exercise-strength-training-b379697dd2290786739ed442d4173cd7)
- A Weekly Workout to Protect Your Knees (https://nytimes.com/2025/09/01/well/move/knee-pain-workout-strength.html)
- Consult Healthcare Providers About Treatment Options
- Doctors respond to ‘data-free’ decision over menopause hormone therapy: ‘It’s not true’ (https://theguardian.com/us-news/2025/nov/24/menopause-hormone-therapy)
- Hormone therapy effective in reducing prevalence of knee osteoarthritis, shows study (https://news-medical.net/news/20190108/Hormone-therapy-effective-in-reducing-prevalence-of-knee-osteoarthritis-shows-study.aspx)
- Hormone Therapy Linked to Reduced Symptomatic Knee OA in Postmenopausal Women (https://endocrinologyadvisor.com/news/hormone-therapy-linked-to-reduced-symptomatic-knee-oa-in-postmenopausal-women)
- A Comprehensive Review of Non-Steroidal Anti-Inflammatory Drug Use in The Elderly - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5772852)
- Joint Pain in Menopause (https://arthritis.org/news/news-and-events/joint-pain-in-menopause)
- Track Symptoms and Progress for Effective Management
- Menopause and Joint Pain | Mass General Brigham (https://massgeneralbrigham.org/en/about/newsroom/articles/menopause-and-joint-pain)
- Joint Pain: An Often Overlooked Symptom of Menopause (https://aarp.org/health/conditions-treatments/menopause-joint-pain)
- Knee pain in menopausal and post menopausal women and non-surgical treatment options (https://caringmedical.com/prolotherapy-news/knee-pain-middle-age-post-menopausal-women)
- Duke Research Sheds Light on Menopause Pain in Oprah Daily | Duke Department of Orthopaedic Surgery (https://ortho.duke.edu/news/dr-jocelyn-wittstein-sheds-light-menopause-pain-oprah-daily)
- Menopause and Joint Pain: An Orthopedic Perspective (https://orthopedicsri.com/blog-items/menopause-and-joint-pain-an-orthopedic-perspective)