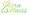Introduction
We understand that navigating the complexities of postmenopausal bleeding (PMB) can be overwhelming for many women. This experience often brings confusion and anxiety, especially when faced with the possibility of serious health issues. Did you know that up to 10% of women who experience PMB may be dealing with significant conditions like endometrial cancer? Recognizing the symptoms and seeking timely medical attention can truly be life-saving.
You are not alone in your worries about cramps and bleeding after menopause. Many women share these concerns, questioning the causes and implications of their symptoms, and wondering when it’s time to seek help. This article is here to support you, offering critical insights into PMB. We aim to equip you with the knowledge needed to navigate this challenging phase of life with confidence and clarity. Together, we can transform uncertainty into understanding.
Define Postmenopausal Bleeding and Its Significance
(PMB) can be a source of worry for many women. It’s defined as any that occurs 12 months or more after your last menstrual period, and it’s important to recognize it as an abnormal condition. This experience can arise from various , including , benign growths like polyps or fibroids, and even more such as . We understand how concerning this can be, as PMB may signal that require .
Recent studies show that up to 10% of women experiencing PMB may have . This statistic underscores the importance of thorough . Gynecologists emphasize that even a single instance of should prompt a conversation with a healthcare provider. can lead to significantly better outcomes. For example, when is caught early, the prognosis is quite favorable, with a 5-year survival rate of 90%.
Real-life stories highlight the that PMB presents, as its from person to person. Healthcare providers often take a , using , transvaginal ultrasounds, and biopsies to uncover the underlying cause of the bleeding. This teamwork among healthcare professionals not only enhances the but also ensures that patients receive timely and appropriate treatment.
In summary, is vital for female health. It can indicate that . By being aware of the symptoms and taking proactive healthcare measures, you can seek the evaluations and interventions you need. Remember, you are not alone in this journey, and we are here to help you improve your .
Identify Common Causes of Postmenopausal Bleeding
can be a distressing experience, and it’s important to understand that you’re not alone in facing this challenge. At , we truly empathize with the emotional and physical toll that can take on your health. Our physician-led approach is designed to provide tailored to your unique needs, ensuring you feel supported every step of the way.
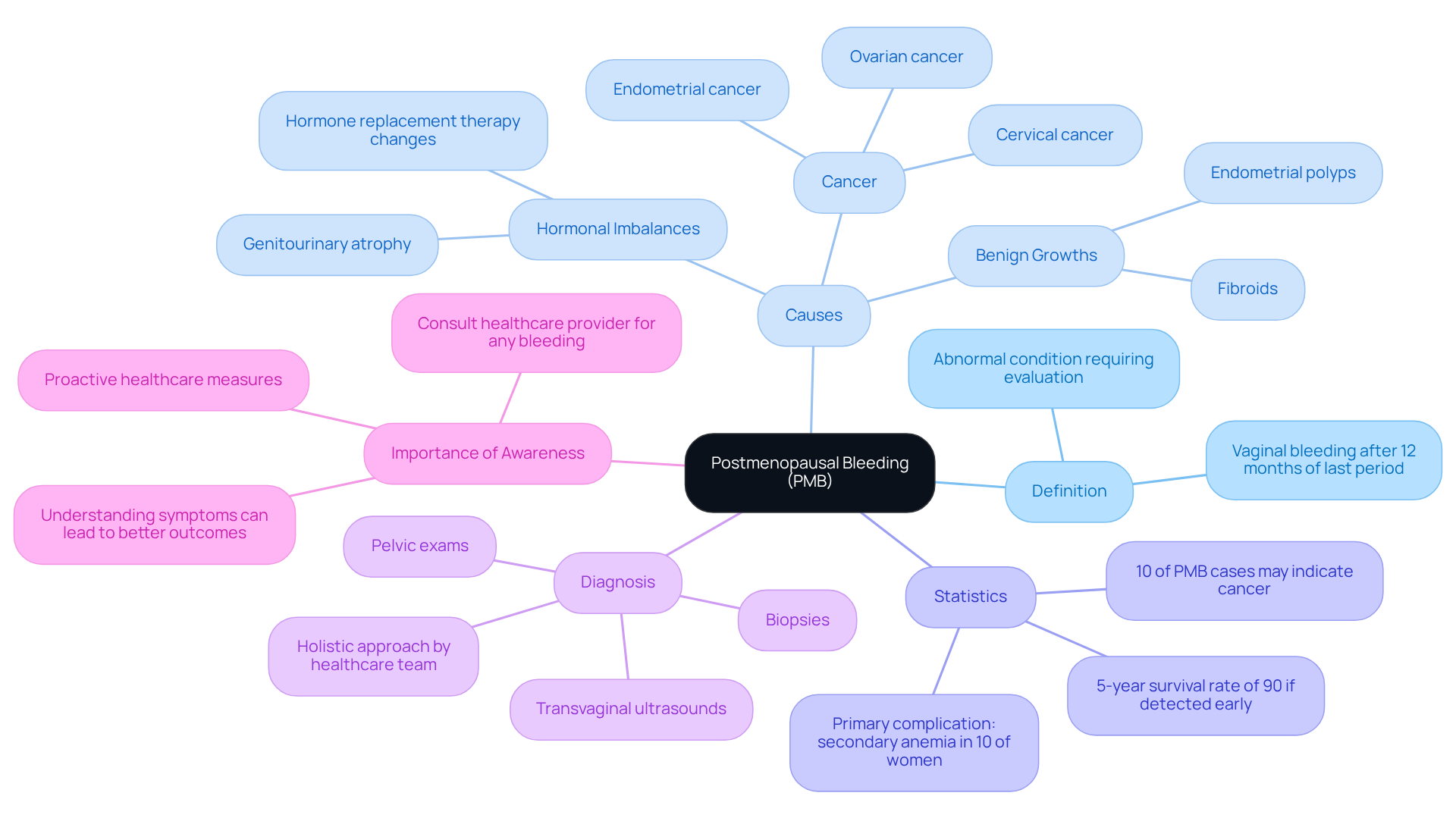
One common cause of is , which occurs when the vaginal walls become thin and inflamed due to decreased estrogen levels. This condition affects up to 60% of , leading to symptoms like dryness, irritation, and that can be exacerbated by everyday activities. At , we offer targeted medical plans that address these symptoms through personalized hormone therapy and holistic support, helping you regain comfort and confidence.
Another contributor is , where the , [potentially causing along with unexpected discharge](https://blog.misrawellness.com/p/146ed02a-9200-431d-b722-be500908519a/). are a frequent consequence of hormonal changes. Our continuous care model is here to monitor and manage these changes effectively, ensuring you feel secure in your health journey.
Polyps, which are [[[noncancerous growths in the uterus or cervix](https://yalemedicine.org/conditions/postmenopausal-bleeding)](https://yalemedicine.org/conditions/postmenopausal-bleeding)](https://yalemedicine.org/conditions/postmenopausal-bleeding), are found in about 30% of PMB cases. While they are usually harmless, they can lead to . At , we conduct comprehensive evaluations to ensure proper management, so you can focus on what truly matters.
It’s also important to consider . Some can result in , which may require adjustments in your treatment plan. Our dedicated team is here to make any necessary modifications promptly, ensuring your comfort and peace of mind.
is another condition that involves and can sometimes progress to cancer if not addressed. for those at risk, and our plans include routine assessments to safeguard your long-term health.
In some cases, may indicate the presence of . , as the is approximately 95% when caught early. At , we prioritize to address any serious conditions, ensuring you receive the care you deserve.
Recognizing these causes is vital for timely intervention and effective treatment. It’s worth noting that about 4-11% of will experience , which can include , at some point, highlighting the prevalence of PMB. The potential outcomes of PMB, including due to anxiety about , are significant and should be taken seriously.
As Dr. Mary Jane Minkin wisely states, "Only your healthcare provider can determine what may be causing ." This underscores the importance of consulting a healthcare professional, like those at , whenever you experience instances of PMB. We are here to help you navigate this journey with compassion and expertise.
Recognize When to Seek Medical Attention
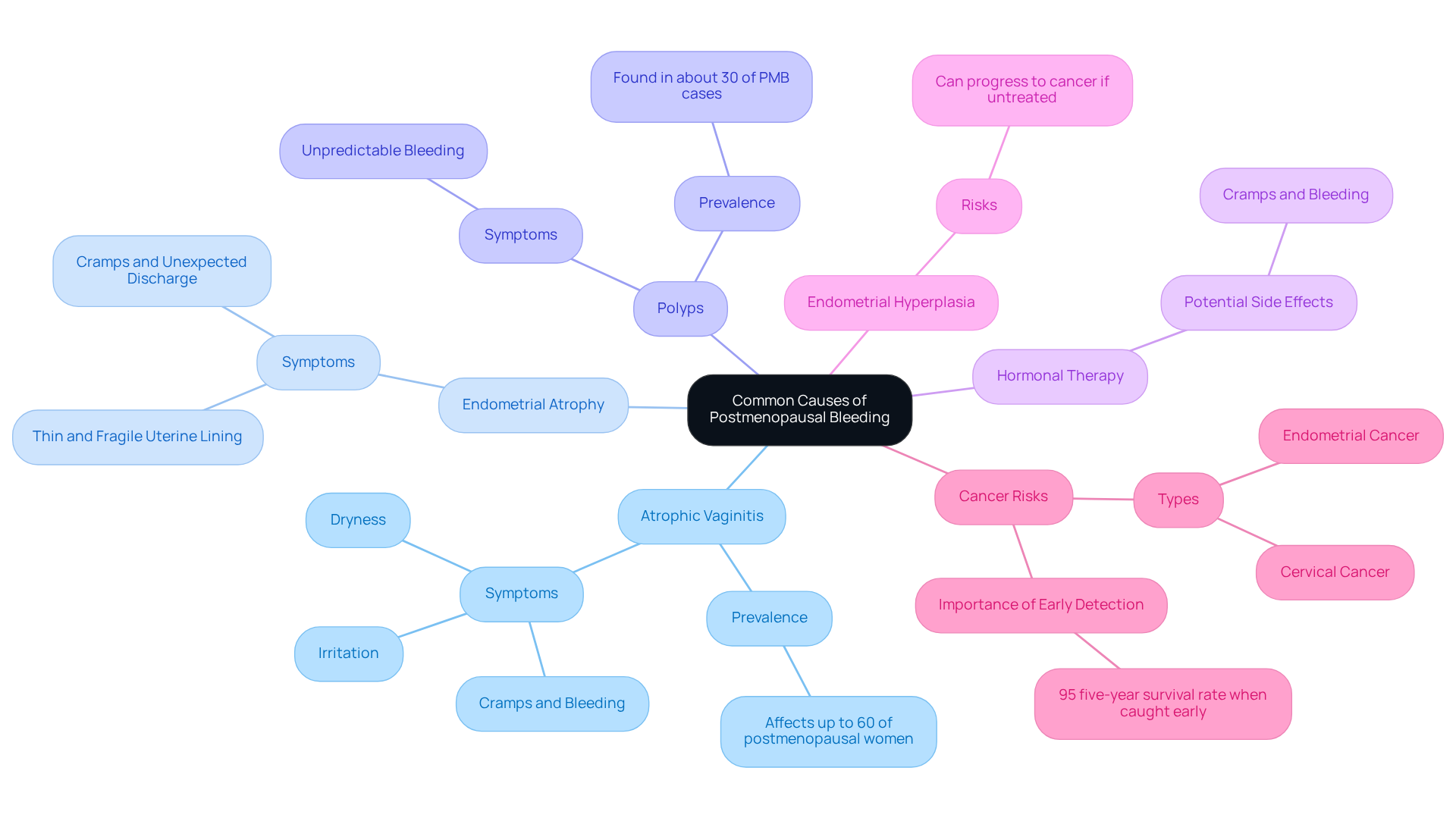
If you’re experiencing any , it’s important to seek medical attention. This can be a sign of , such as uterine cancer, especially if you're experiencing , and we understand how concerning this can be. , along with , may indicate more serious conditions like uterine polyps or fibroids. If you’re also facing , such as , please don’t hesitate to get evaluated right away. Additional symptoms such as unexplained weight loss, fatigue, or changes in bowel or urinary habits can also be associated with significant .
At , we recognize that these symptoms can deeply affect your quality of life. We’re here to help you navigate this challenging time. Our for include:
- Discussions about both hormonal and non-
is crucial to rule out severe conditions, including , particularly for women experiencing , which affects about 10% of them. Healthcare providers often recommend to pinpoint the cause of the discharge.
By recognizing these symptoms and acting swiftly, you can lead to timely interventions that improve outcomes and ensure comprehensive care. Remember, you are not alone in this journey. We are here to every step of the way.
Understand the Diagnostic Process for Postmenopausal Bleeding
At , we understand that experiencing can be a source of anxiety and concern. That’s why our diagnostic process is designed with your comfort and well-being in mind, ensuring a thorough evaluation and compassionate management every step of the way.
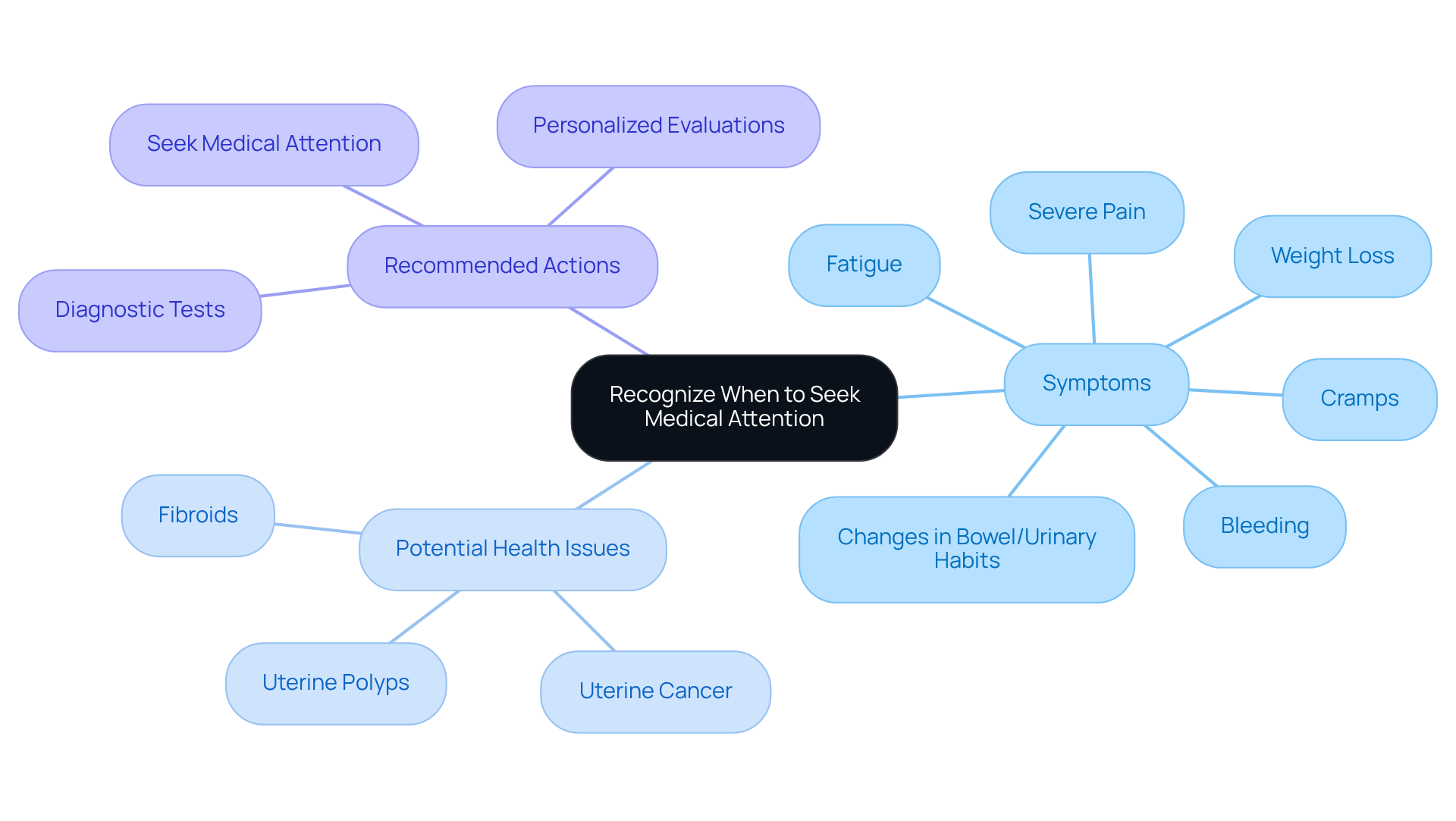
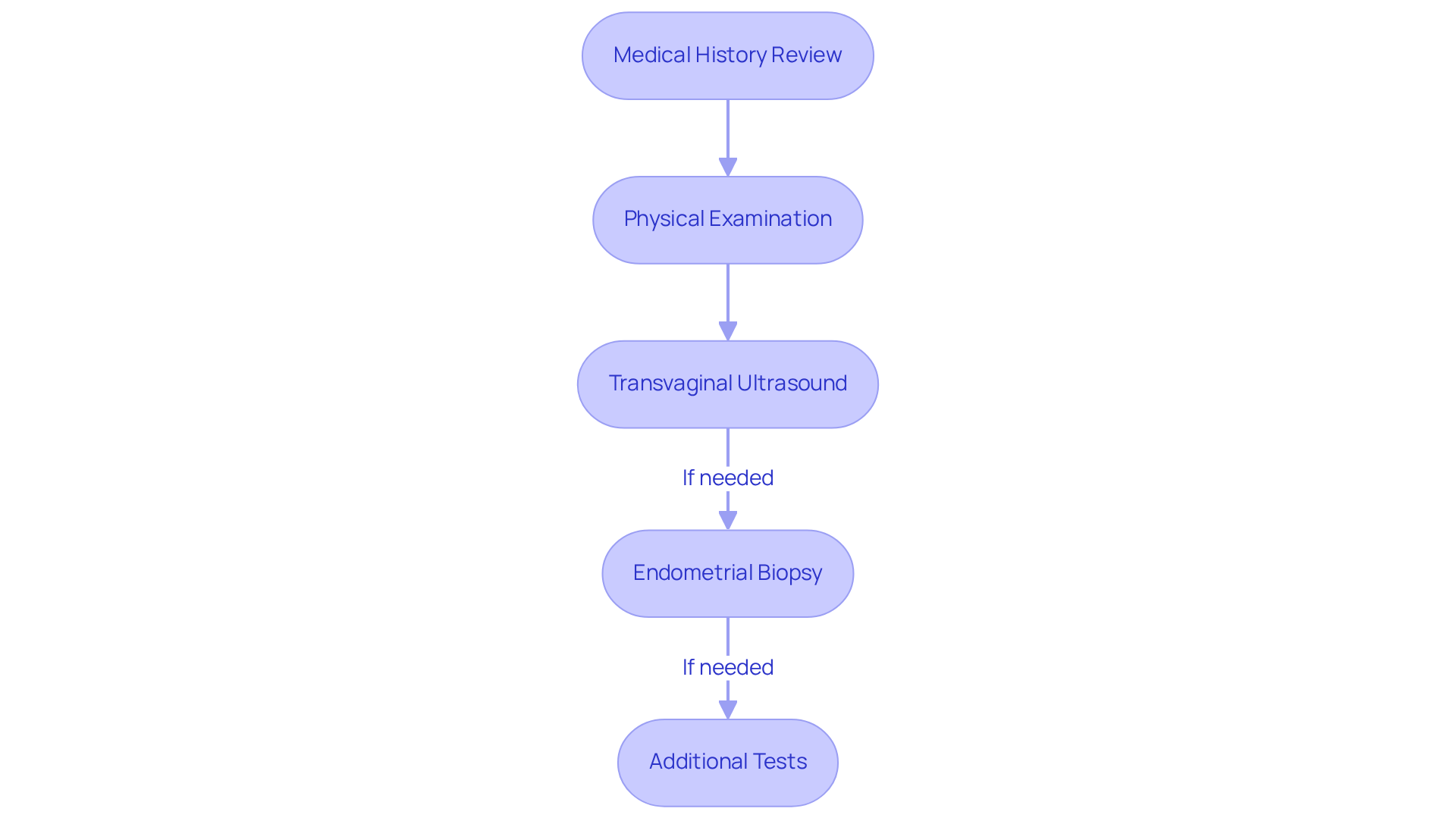
- Medical History Review: We begin with a heartfelt discussion about your symptoms, medical history, and current medications. This vital information helps our healthcare providers identify any potential risk factors and underlying conditions, allowing us to create a tailored just for you.
- Physical Examination: A is conducted to check for any abnormalities. This initial step provides crucial insights into your , setting the stage for effective management.
- Transvaginal Ultrasound: This imaging technique plays a key role in assessing the uterus and ovaries for any abnormalities. Research shows that , boasting a high negative predictive value for ruling out uterine cancer and identifying conditions like fibroids and endometrial polyps. In fact, 3D ultrasound outperforms 2D technology in pinpointing the causes of , ensuring you receive the most accurate diagnostics available.
- Endometrial Biopsy: If needed, we may take a sample of the uterine lining to check for cancerous cells. This step is crucial, as are a presenting indication in over 90% of individuals with uterine cancer, highlighting the [[[[importance of prompt assessment](https://pmc.ncbi.nlm.nih.gov/articles/PMC10490884)](https://pmc.ncbi.nlm.nih.gov/articles/PMC10490884)](https://pmc.ncbi.nlm.nih.gov/articles/PMC10490884)](https://pmc.ncbi.nlm.nih.gov/articles/PMC10490884).
- Additional Tests: Depending on what we find in the earlier steps, further tests may be necessary, such as blood tests or hysteroscopy, to gain a complete understanding of your condition.
can help you prepare for your appointment and actively participate in your healthcare journey at our . We cannot stress enough how important is; . It’s worth noting that statistics reveal disparities in care quality, with 77.1% of Medicaid patients and 87.4% of commercially insured patients receiving a after the index PMB.
As Dr. Steven Goldstein wisely states, "Performing ultrasound first on women who present with is sound judgment for gynecologists." At our , we are dedicated to providing affordable and , all aimed at improving the quality of care for our patients. Remember, you are not alone in this journey; we are here to help.
Explore Management and Treatment Options
For many women, experiencing cramps and can be a distressing and confusing time. At , we understand the , and we’re here to help you navigate through it with care and compassion.
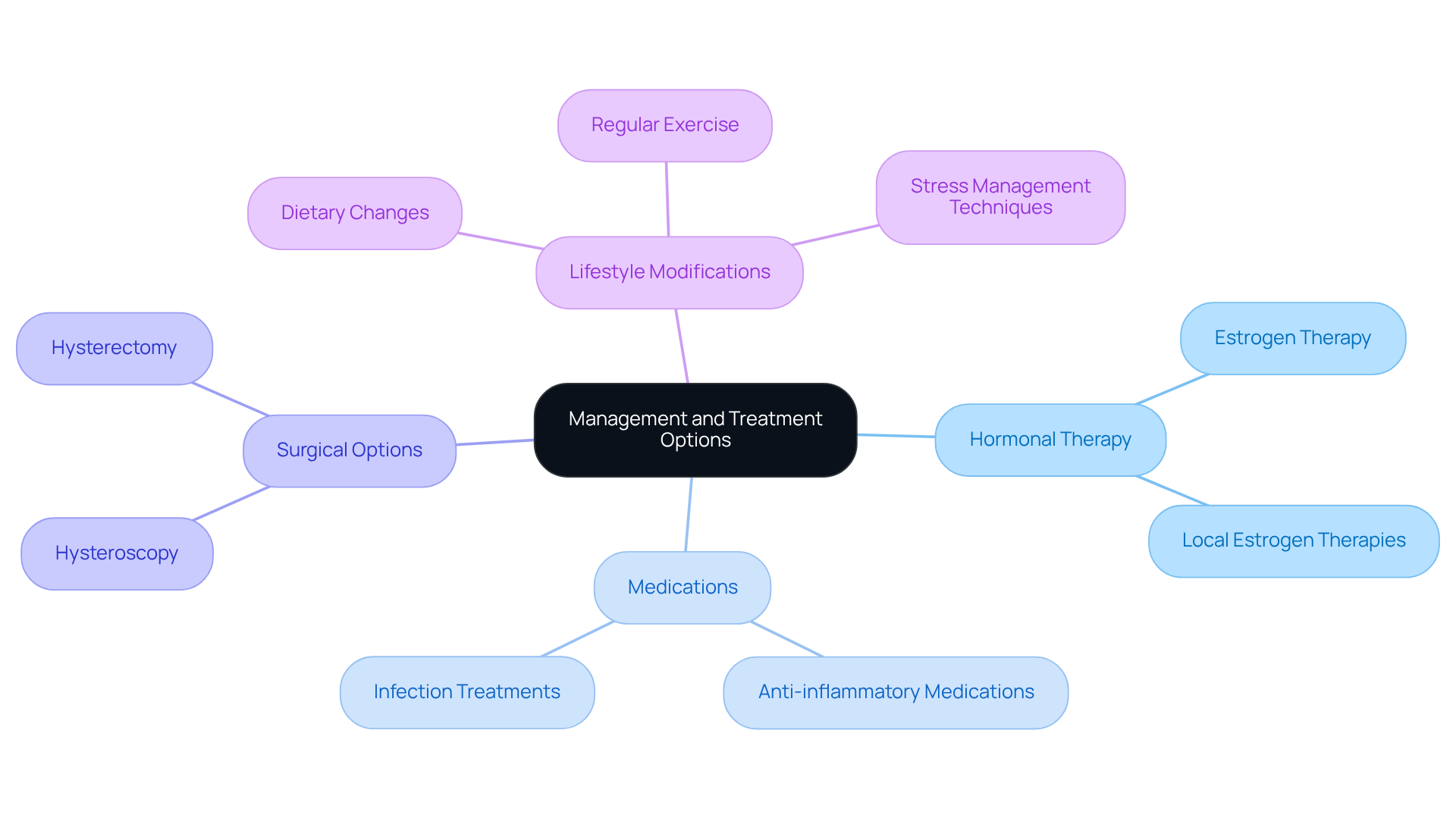
: For those struggling with symptoms related to atrophic vaginitis and endometrial atrophy, estrogen therapy can provide significant relief. Recent conversations among gynecologists have highlighted the safety and benefits of , especially after the . This shift reflects a growing consensus among healthcare professionals about the safety of local estrogen therapies, which can enhance overall health outcomes for menopausal women. At our wellness center, we focus on personalized as part of a comprehensive management strategy, ensuring that your hormonal balance and long-term health are prioritized.
Medications: We also recognize that can play a vital role in managing symptoms or addressing underlying conditions, such as metabolic disorders and thyroid issues. Medications aimed at reducing inflammation or treating infections may be prescribed to help prevent hemorrhage. At , we take a holistic approach, blending standard and alternative treatments to optimize your health outcomes.
Surgical Options: In cases where bleeding is severe or persistent, . Procedures like or a hysterectomy can effectively address the root causes of bleeding, ultimately improving your quality of life. We provide continuous clinical follow-up to ensure you receive the essential support throughout your treatment journey.
Lifestyle Modifications: Making dietary changes, engaging in regular exercise, and practicing stress management techniques can significantly enhance your overall health and hormonal balance. We encourage you to discuss these options with your healthcare provider to create a that aligns with your specific symptoms and health goals. At , we believe that and lifestyle evaluations are key components of your care, empowering you to take charge of your well-being.
Understanding these management strategies is crucial for anyone facing . Prompt intervention can lead to improved health outcomes and a better quality of life. It’s important to remember that between 10% and 15% of women experiencing cramps and might have endometrial cancer. Therefore, if you notice any bleeding more than a year after your last menstrual period, please consult a healthcare provider. You are not alone in this journey, and we are here to support you every step of the way.
Conclusion
Understanding the complexities of postmenopausal bleeding (PMB) is crucial for women's health. This experience can be daunting, often signaling serious underlying conditions that require immediate medical attention. We understand that any vaginal bleeding after menopause can be concerning, and recognizing its significance is the first step toward taking charge of your health. By being aware, you can ensure that you receive the necessary evaluations and treatments.
This article has explored the various causes of cramps and bleeding after menopause, from hormonal changes to benign growths and even potential cancers. It’s vital to emphasize the importance of timely medical assessments, such as pelvic exams and imaging tests, to accurately diagnose and manage these symptoms. Remember, you are not alone in this journey. Compassionate, personalized care is available to support you through this challenging phase of life.
Ultimately, awareness and education about postmenopausal symptoms empower you to seek help when needed. Taking charge of your health by consulting healthcare providers at the first sign of unusual bleeding or discomfort can lead to better outcomes and an improved quality of life. Addressing these symptoms promptly is not just about managing discomfort; it can be a critical step in safeguarding your long-term health and well-being. We are here to help you navigate this path.
Frequently Asked Questions
What is postmenopausal bleeding (PMB)?
Postmenopausal bleeding (PMB) is defined as any vaginal bleeding that occurs 12 months or more after a woman's last menstrual period. It is considered an abnormal condition that may indicate various health issues.
What are some potential causes of PMB?
Potential causes of PMB include hormonal imbalances, benign growths such as polyps or fibroids, Atrophic Vaginitis, Endometrial Atrophy, hormonal therapy effects, Endometrial Hyperplasia, and more serious conditions like endometrial or cervical cancer.
Why is PMB significant?
PMB is significant because it may signal serious medical issues that require prompt evaluation and care. Studies show that up to 10% of women experiencing PMB may have endometrial or uterine cancer, highlighting the importance of early detection.
What should a woman do if she experiences PMB?
If a woman experiences PMB, it is crucial to consult a healthcare provider, even if it is a single instance of bleeding. Early detection and evaluation can lead to better health outcomes.
How is PMB diagnosed?
PMB is diagnosed through a comprehensive approach that may include pelvic exams, transvaginal ultrasounds, and biopsies to uncover the underlying cause of the bleeding.
What is Atrophic Vaginitis and how does it relate to PMB?
Atrophic Vaginitis is a condition where the vaginal walls become thin and inflamed due to decreased estrogen levels, affecting up to 60% of postmenopausal women. It can cause symptoms like dryness, irritation, and cramps, which may lead to bleeding.
What role do polyps play in PMB?
Polyps are noncancerous growths found in the uterus or cervix, present in about 30% of PMB cases. While usually harmless, they can lead to unpredictable bleeding.
How can hormonal therapy affect postmenopausal bleeding?
Some hormone replacement therapies may result in cramps and bleeding after menopause, which could necessitate adjustments in the treatment plan.
What is Endometrial Hyperplasia and its significance in PMB?
Endometrial Hyperplasia involves the thickening of the uterine lining and can potentially progress to cancer if not addressed. Regular monitoring is essential for those at risk.
What are the implications of experiencing unexpected spotting after menopause?
About 4-11% of postmenopausal women may experience unexpected spotting, which can indicate PMB. It is important to take these occurrences seriously due to potential risks such as anemia or anxiety affecting intimacy.
List of Sources
- Define Postmenopausal Bleeding and Its Significance
- Postmenopausal Bleeding - StatPearls - NCBI Bookshelf (https://ncbi.nlm.nih.gov/books/NBK562188)
- Postmenopausal Bleeding (https://yalemedicine.org/conditions/postmenopausal-bleeding)
- Postmenopausal Bleeding (https://my.clevelandclinic.org/health/diseases/21549-postmenopausal-bleeding)
- Life-Saving Advice About Postmenopausal Bleeding - Physician Resources | Fox Chase Cancer Center (https://physicianresources.foxchase.org/videos/life-saving-advice-about-postmenopausal-bleeding)
- Identify Common Causes of Postmenopausal Bleeding
- Postmenopausal Bleeding Causes: 10 Essential Alarming Facts 2025 (https://southlakeobgyn.net/2025/06/27/postmenopausal-bleeding-causes)
- Postmenopausal Bleeding (https://my.clevelandclinic.org/health/diseases/21549-postmenopausal-bleeding)
- Postmenopausal Bleeding (https://yalemedicine.org/conditions/postmenopausal-bleeding)
- Recognize When to Seek Medical Attention
- Bleeding after menopause: It’s not normal | Cancer | UT Southwestern Medical Center (https://utswmed.org/medblog/postmenopausal-bleeding)
- Is postmenopausal bleeding a concern? (https://mayoclinichealthsystem.org/hometown-health/speaking-of-health/postmenopausal-bleeding-should-you-be-concerned)
- Postmenopausal Bleeding (https://yalemedicine.org/conditions/postmenopausal-bleeding)
- Postmenopausal Bleeding (https://my.clevelandclinic.org/health/diseases/21549-postmenopausal-bleeding)
- Life-Saving Advice About Postmenopausal Bleeding - Physician Resources | Fox Chase Cancer Center (https://physicianresources.foxchase.org/videos/life-saving-advice-about-postmenopausal-bleeding)
- Understand the Diagnostic Process for Postmenopausal Bleeding
- Identifying the Causes of Postmenopausal Bleeding (https://volusonclub.net/empowered-womens-health/identifying-the-causes-of-postmenopausal-bleeding)
- Timeliness of diagnostic evaluation for postmenopausal bleeding: A retrospective cohort study using claims data - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10490884)
- Explore Management and Treatment Options
- FDA reverses decades-old warning on hormone therapy products for menopause (https://statnews.com/2025/11/10/fda-reverses-hormone-warning-menopause-health)
- Postmenopausal Bleeding (https://my.clevelandclinic.org/health/diseases/21549-postmenopausal-bleeding)
- Postmenopausal Bleeding (https://yalemedicine.org/conditions/postmenopausal-bleeding)
- HHS Advances Women’s Health, Removes Misleading FDA Warnings on Hormone Replacement Therapy (https://fda.gov/news-events/press-announcements/hhs-advances-womens-health-removes-misleading-fda-warnings-hormone-replacement-therapy)