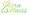Introduction
As women navigate the journey through menopause, they often face a challenging mix of hormonal changes that can deeply affect their well-being, especially when it comes to migraines. With estrogen levels fluctuating and sometimes dropping sharply, many find themselves grappling with an increase in both the frequency and intensity of these painful headaches. We understand how overwhelming this can be.
This article explores the vital connection between migraines and menopause, shedding light on the underlying causes and sharing effective treatment strategies that can help women reclaim their quality of life. You are not alone in this struggle, and as we delve into the risks associated with these migraines intertwined with other health concerns, we are here to help you navigate this complex landscape to find relief and support.
Explore the Connection Between Migraines and Menopause
Migraines with menopause can be a heavy burden, particularly for those undergoing hormonal changes. As estrogen levels dip, many find themselves grappling with more frequent and intense migraines with menopause. It’s a struggle that can feel isolating, but you are not alone. Research shows that these hormonal shifts can alter headache patterns, making it crucial for women to recognize the connection between their headaches and migraines with menopause. In fact, studies reveal that women are three times more likely to suffer from migraines with menopause than men, and this disparity often intensifies during the menopausal transition.
Imagine navigating this challenging time, only to discover that severe headaches and other symptoms can increase your risk of heart disease and stroke. A systematic review found that those facing both severe headaches and vasomotor issues during this transition are at a 1.5 times higher risk for heart disease and a 1.7 times higher risk for stroke compared to those with fewer issues. While these risks can decrease when considering traditional cardiovascular factors, the emotional toll can still be significant.
At [[[[Misra Wellness](https://misrawellness.com)](https://misrawellness.com)](https://misrawellness.com)](https://misrawellness.com), we understand the importance of a thorough evaluation for treatment eligibility. We believe in combining your symptoms, medical history, and clinical insight to create personalized care plans tailored just for you. We are here to help you navigate this transition with compassion and expertise.
However, it’s important to note that research on headaches worsening after the reproductive phase has shown mixed results, reflecting the varied experiences of individuals. Recognizing these patterns can empower you to seek the right treatment and support, ultimately enhancing your quality of life during this phase. Remember, you don’t have to face this alone; we’re here to support you every step of the way.
Identify Causes of Migraines During Menopause
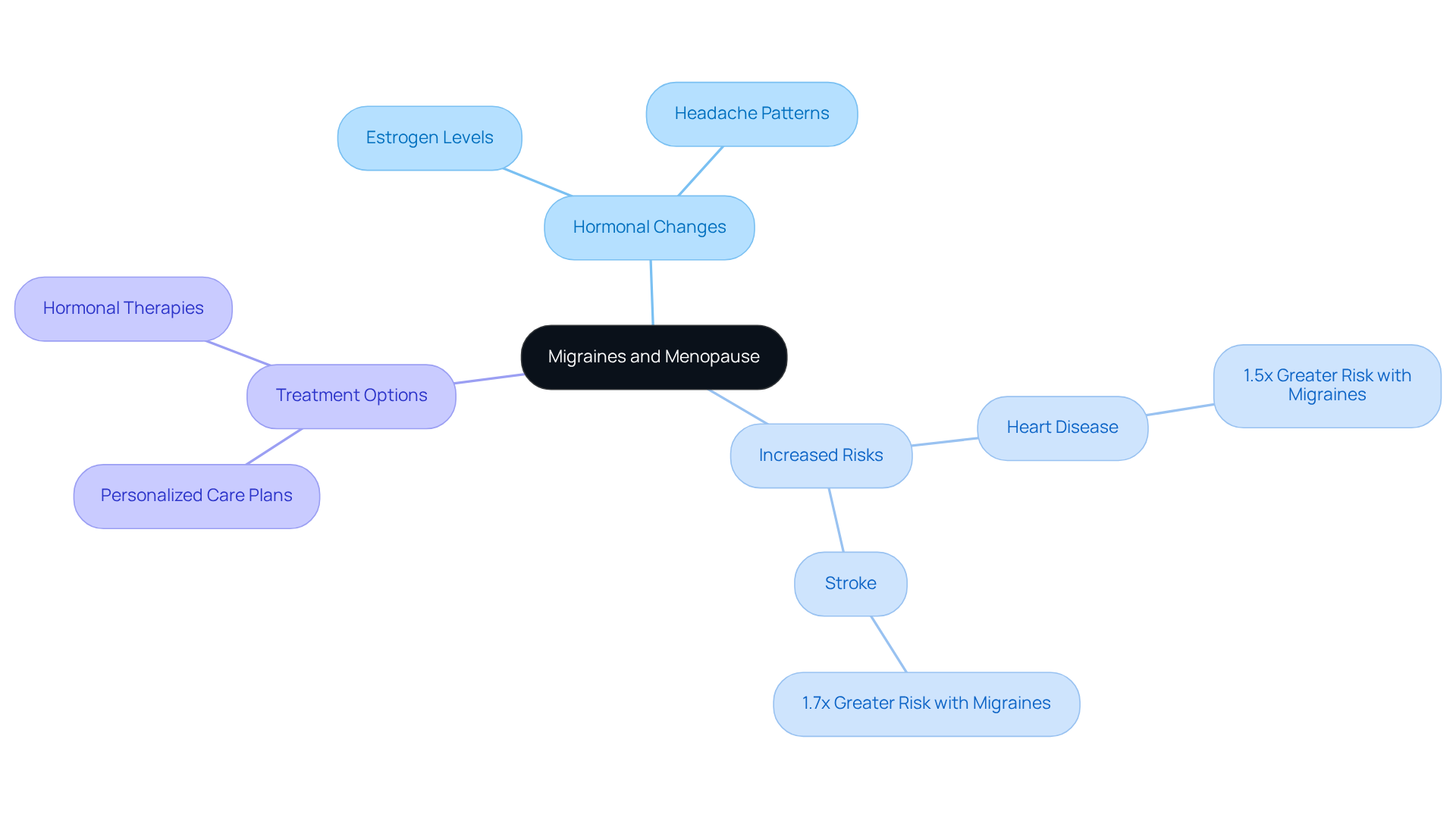
Many women face the challenge of migraines during their transition, and we understand how overwhelming this can be. Hormonal fluctuations, particularly the decrease in estrogen levels, often trigger more frequent and severe headaches. Research shows that during this transitional phase, the risk of experiencing high-frequency headaches can rise dramatically - by as much as 76 percent among women.
Alongside these hormonal changes, heightened stress levels during menopause can intensify headache symptoms. When cortisol levels rise, they can disrupt [[[[hormonal balance](https://misrawellness.com)](https://misrawellness.com)](https://misrawellness.com)](https://misrawellness.com), leading to even more intense headaches. Additionally, dietary changes - whether intentional or driven by cravings - can also provoke headaches. Common culprits include foods rich in tyramine, caffeine, and alcohol. It’s essential to manage stress and make mindful dietary choices to help reduce the frequency of headaches.
Sleep disturbances are another significant factor. Many individuals notice disruptions in their sleep patterns during this stage of life, and poor sleep quality is closely linked to headache disorders, contributing to an increase in headache frequency. Moreover, some medications used to manage symptoms related to hormonal changes may inadvertently trigger severe headaches. It’s crucial to discuss all medications with your healthcare provider to identify any potential side effects.
At [[[[Misra Wellness](https://misrawellness.com)](https://misrawellness.com)](https://misrawellness.com)](https://misrawellness.com), we offer a comprehensive membership plan designed to help manage symptoms associated with this life stage. Our personalized care addresses these interconnected factors, empowering women to seek suitable care and develop effective strategies for handling headaches. As Dr. Vincent Martin wisely notes, 'Women have been informing physicians that their headache episodes, including migraines with menopause, worsen around this time, and now we have evidence they were correct.' We are here to help, providing physician-led support for hormonal balance and enhancing your quality of life through our Direct Primary Care model.
Implement Treatment Strategies for Menopausal Migraines
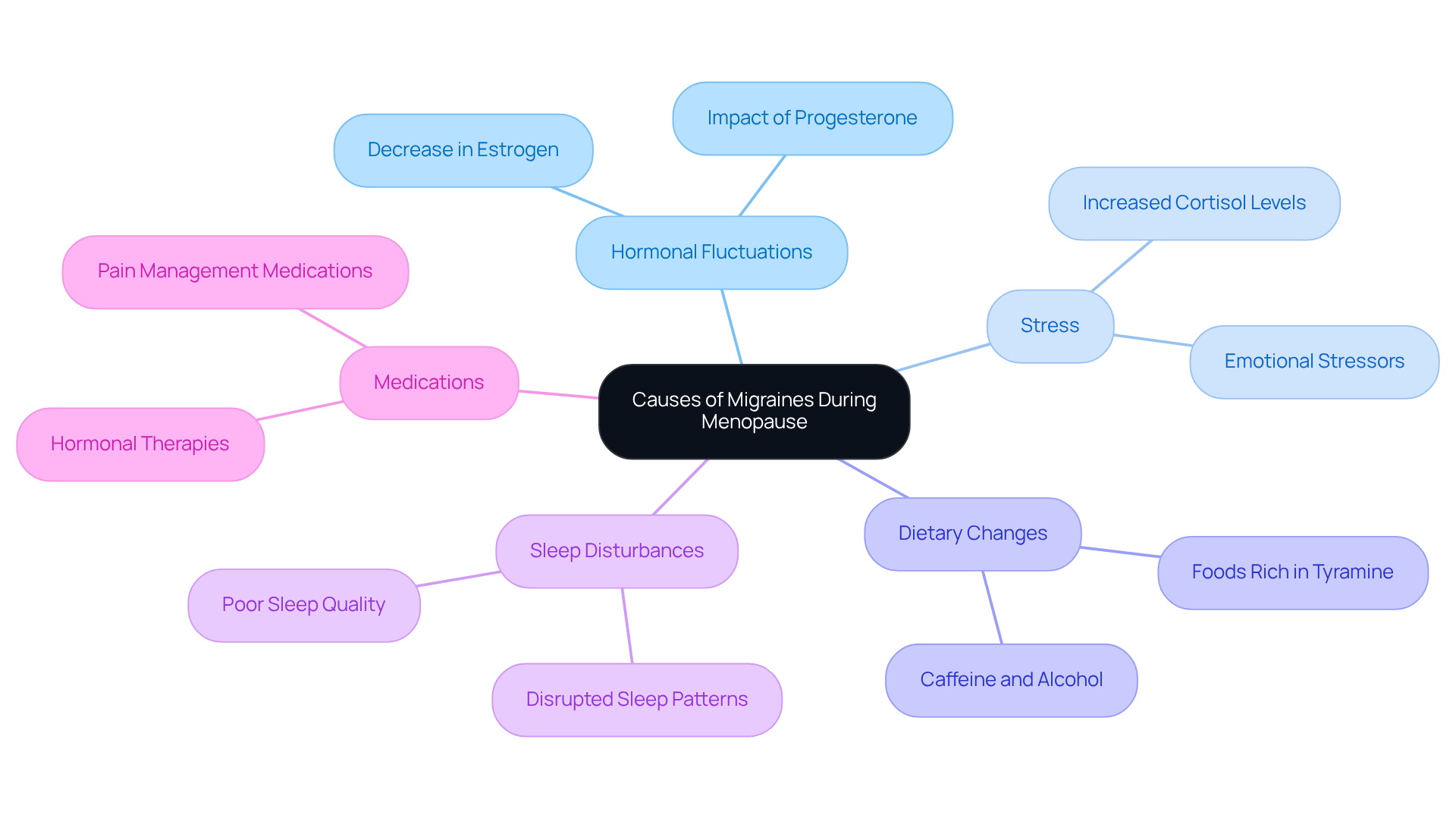
Lifestyle Modifications:
- Regular Exercise: We understand that migraines can be debilitating. Engaging in regular physical activity can significantly reduce the frequency and severity of these headaches. Aim for at least 30 minutes of moderate exercise most days of the week. Research shows that aerobic exercise can decrease headache days by 22% to 78% for those suffering from migraines with menopause. Dr. Dana Ionel reminds us, "Exercise releases endorphins, which are the body’s natural painkillers," making it a beneficial strategy for managing headaches.
- Healthy Diet: A balanced diet rich in fruits, vegetables, whole grains, and healthy fats is essential for your well-being. It’s important to avoid known triggers for headaches, such as aged cheeses, processed meats, and excessive caffeine.
- Stress Management: You are not alone in feeling overwhelmed. Incorporating stress-reducing techniques like yoga, meditation, or deep-breathing exercises into your daily routine can help alleviate triggers and bring you peace.
- Sleep Hygiene: Establishing a regular sleep schedule and creating a restful environment can enhance your sleep quality, which is crucial for managing headaches.
- Medications: Consult with a healthcare provider about suitable treatments for headache management. Options may include:
- Preventive Medications: Such as beta-blockers, antidepressants, or anticonvulsants, which can help reduce the frequency of migraines. Non-hormonal medications like venlafaxine and clonidine have also proven effective for managing both migraines with menopause and other related issues. Dr. Ionel emphasizes, "Before starting an exercise program, it’s important to check with your doctor," highlighting the need for professional guidance.
- Acute Treatments: Triptans and NSAIDs can be effective for addressing headache attacks when they occur.
- Hormone Replacement Therapy (HRT): For some women, HRT may alleviate menopausal symptoms and potentially decrease the frequency of migraines with menopause. However, it’s crucial to discuss the risks and benefits with a healthcare provider, as some may experience aggravated headaches with HRT. At Misra Wellness, we offer personalized menopause care plans through our Direct Primary Care model, considering these factors to enhance your quality of life.
- Alternative Therapies: Consider complementary approaches such as acupuncture, biofeedback, or dietary supplements like magnesium and riboflavin, which have shown promise in preventing headaches. Vaginal preparations containing oestrogen can also alleviate menopausal symptoms without affecting migraine conditions, as the oestrogen is not absorbed into the bloodstream.
Conclusion
Navigating the challenges of migraines during menopause can feel overwhelming, and it’s important to recognize the significant connection between hormonal changes and the increase in headache frequency. As estrogen levels decline, many women find themselves facing intensified migraine symptoms. Understanding these shifts is crucial, as it empowers women to seek the support and treatment they need during this transitional phase.
Key insights reveal that the causes of migraines in menopausal women are multifaceted. Hormonal fluctuations, stress, dietary changes, and sleep disturbances all play a role. By making lifestyle modifications - like incorporating regular exercise, maintaining a balanced diet, and practicing effective stress management techniques - individuals may find relief from the severity and frequency of their migraines. Additionally, exploring medical treatments, such as preventive medications and hormone replacement therapy, can be vital in managing symptoms.
Ultimately, addressing migraines during menopause goes beyond just alleviating pain; it’s about enhancing your overall quality of life. If you’re experiencing these challenges, know that you’re not alone. Seeking personalized care and support is essential, and you deserve to navigate this life stage with confidence and well-being. Taking proactive steps today can lead to a healthier tomorrow, highlighting the importance of informed decision-making in managing menopausal migraines. We are here to help you every step of the way.
Frequently Asked Questions
How are migraines related to menopause?
Migraines can become more frequent and intense during menopause due to hormonal changes, particularly the decline in estrogen levels. Research indicates that women are three times more likely to experience migraines during menopause compared to men, with this disparity increasing during the menopausal transition.
What risks are associated with severe headaches during menopause?
Women experiencing severe headaches along with vasomotor symptoms during menopause face higher health risks. A systematic review found that they are 1.5 times more likely to develop heart disease and 1.7 times more likely to suffer a stroke compared to those with fewer symptoms.
What support is available for women dealing with migraines and menopause?
Misra Wellness emphasizes the importance of a thorough evaluation to create personalized care plans. They combine symptoms, medical history, and clinical insights to help women navigate the challenges of menopause, including migraines, with compassion and expertise.
Is there consistent research on headaches worsening after the reproductive phase?
Research on the worsening of headaches after the reproductive phase shows mixed results, indicating that experiences can vary among individuals. Recognizing these patterns can help women seek appropriate treatment and support.
How can understanding the connection between migraines and menopause improve quality of life?
By recognizing the link between migraines and menopause, women can seek the right treatment and support, which can enhance their overall quality of life during this transitional phase.
List of Sources
- Explore the Connection Between Migraines and Menopause
- Migraines Worsen As Women Approach Menopause (https://uc.edu/news/articles/legacy/healthnews/2016/01/migraines-worsen-as-women-approach-menopause.html)
- Hot flashes plus migraines ups risk of heart disease and stroke after menopause (https://nhlbi.nih.gov/news/2024/hot-flashes-plus-migraines-ups-risk-heart-disease-and-stroke-after-menopause)
- Patterns of Migraine in Postmenopausal Women: A Systematic Review - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC7989683)
- Migraine in Women Peaks Around Menopause, Declines With Advancing Age (https://sleepwakeadvisor.com/news/migraine-in-women-peaks-around-menopause-declines-with-advancing-age)
- Menopause and migraines: New findings point to power of prevention (https://michiganmedicine.org/health-lab/menopause-and-migraines-new-findings-point-power-prevention)
- Identify Causes of Migraines During Menopause
- Migraines Worsen As Women Approach Menopause (https://uc.edu/news/articles/legacy/healthnews/2016/01/migraines-worsen-as-women-approach-menopause.html)
- Women's Day 2026: Why Migraines And Stroke Risk Are Higher In Women (https://ndtv.com/health/womens-day-2026-why-migraines-and-stroke-risk-are-higher-in-women-11180711)
- Patterns of Migraine in Postmenopausal Women: A Systematic Review - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC7989683)
- Implement Treatment Strategies for Menopausal Migraines
- Review Find Moderate Evidence That Aerobic Exercise Lowers Number of Migraine Days | AJMC (https://ajmc.com/view/review-find-moderate-evidence-that-aerobic-exercise-lowers-number-of-migraine-days)
- Migraine and menopause - The Migraine Trust (https://migrainetrust.org/live-with-migraine/migraine-and-menopause)
- Migraine and Exercise | American Migraine Foundation (https://americanmigrainefoundation.org/resource-library/migraine-and-exercise-benefits)
- HRT for Menopausal Migraine (https://webmd.com/migraines-headaches/features/hrt-migraines-menopause)